By Josephat Chiripanyanga
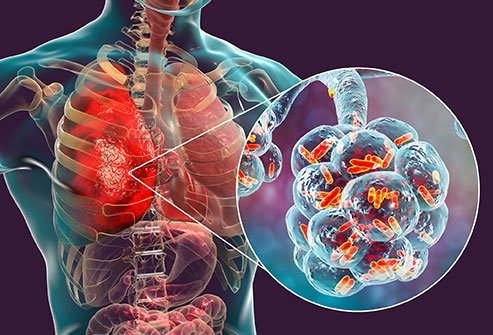
PNEUMONIA is an inflammatory condition of the lungs which mainly affects the alveoli.
The alveolus is the functional tissue of the lung that deals with gaseous exchange. As we all know the primary function of the lung is respiration, which simply put is the inhalation of oxygen and exhalation of carbon dioxide. So this gaseous exchange whereby oxygen is taken into the body and carbon dioxide is sent outside the body occurs in the alveoli. When there is inflammation of the alveoli then one develops pneumonia.
Inflammation is the body’s response to an insult and is signified by the presence of any or all of the cardinal signs of inflation that is pain, heat, redness, swelling and loss of function. So once there is inflammation of the alveoli then pneumonia develops. Once you understand this you will easily understand the symptoms of pneumonia and eventually its treatment and how to avoid or minimize your chances of developing pneumonia.
When it comes to prevalence, pneumonia affects about seven percent of the world population annually. That comes to about 450 million people per year. The mortality rate stands at about one percent. That means one percent of all the people that develop pneumonia will die from it.
This one percent translates to about four million people per year who die from pneumonia. Pneumonia kills a significant number of people per year and as such we need to avoid it and prevent it as much as possible.
The cause for pneumonia is mainly infections. The chief culprits being bacterial infections, followed by viral infections, and rarely fungal or parasitic infections. You can either inhale the bacteria from someone who is coughing and has pneumonia or you can touch your nostrils with hands contaminated with any of these bugs. There are more than a hundred pathogens that can cause pneumonia.
There are a few very rare conditions that result in pneumonia without an infection from any of the pathogens we discussed above. One such example is lymphocytic interstitial pneumonia.
Most pneumonia is community acquired pneumonias. This simply means they were acquired in the community from one individual to the next. Some pneumonias are nosocomial meaning they were acquired in a hospital setting. Community acquired pneumonias are usually easy to treat compared to hospital acquired because the latter is mainly caused by bugs that have been exposed to some antibiotics before and are now resistant to the common antibiotics we normally use to treat the pneumonia.
There are also risk factors to pneumonia. Smoking is a major risk factor. We see that people who smoke tobacco have an increased chance of developing pneumonia. Individuals who are immunocompromised for any reason have a high chance of catching pneumonia. Be it immunocompromisation from HIV/AIDS, diabetes mellitus, cancer, malnutrition in children, obesity in adults, liver disease or simple aging, they all increase the risk of contracting pneumonia.
The symptoms of pneumonia follow from the pathogenesis of the disease. Like we said in the paragraphs at the top, pneumonia occurs because of inflammation of the alveoli. Because the alveoli get blocked by the inflammatory exudate you want to cough it out. And the alveoli are in the lungs which are in the chest cavity you will develop chest pain. Because when there is inflammation there is heat production you will develop a fever. Temperatures can go up. Because you are not getting adequate oxygen into the body you get tired easily and develop fatigue and generalized body weakness. Since you are struggling to get carbon dioxide out of the body your respiratory rate will go faster to try and push carbon dioxide out of the body and you end up short of breath.
When we examine you now for the signs, your pulse will be high, your blood pressure will be low and your respiratory rate will be high. When we auscultate your chest using a stethoscope we can hear diminished or absent breath sounds with crepitations.
With these signs and symptoms we can make a diagnosis of pneumonia. However it’s always best to confirm the diagnosis with a chest Xray. Rarely do we need to do a CT scan to diagnose pneumonia. An ultrasound scan of the chest could be an added advantage in certain cases.
To finally delineate between bacterial and viral pneumonia is usually a difficult task. Mainly it’s what we see from your history and examination that leads us to deciding which type of organism it could be. To finally zero in on one particular bug normally we will need to take your sputum to the laboratory for microscopy, culture and sensitivity. Rarely do we need to do a test called a bronchoscopy and take some aspirates from the lungs and send them to the laboratory.
Treatment is mainly guided by the type of pathogen we are dealing with. If it’s bacterial pneumonia then we just give you a course of antibiotics for a week normally you will be ok. Viral pneumonias will just need some antiviral drugs for a week or so as well. The more stubborn ones are the fungal pneumonias and parasitic pneumonias that would need longer duration of treatment with the antifungals or anti-parasitic agents. Some could even require treatment for life like cryptococcal pneumonia.
So to minimise your chances of contracting pneumonia, avoid smoking, avoid dusty environments and reduce air pollution, get vaccinated against common pathogens that cause pneumonia, get proper treatment of any underlying condition like HIV/AIDS, diabetes mellitus and malnutrition. Wearing face masks, practicing social distancing and avoiding touching your nose.
Since we are in the Covid-19 pandemic era, I also would like to remind you that the pandemic is a type of pneumonia that can also be combated by the above measures, including vaccination. As such I urge you all to go out there and get vaccinated.
Remember a healthy you, a healthy me to a healthy world.
Josephat Chiripanyanga is a Harare-based medical doctor. He can be contacted at joechiripanyanga@gmail.com